Good Physician-Patient Communication – Why is this crucial?
Excellent communication is learned and developed over time and it plays a vital role in understanding the patient’s suffering, establishing the correct diagnosis and prescribing the right treatment which will essentially cure the patient’s illness.
You may be inclined to think communication between two people is something natural and you don’t need specialized training for doing it well. But still, a lot of physicians are struggling with proper communication between them and their patients. Focused on their work with a high attention to details not to miss anything, doctors may overlook the explanation part of their jobs and give the patient an incomplete talk about their condition.
First consultation
The quality of the information obtained by the doctor during the first consultation is closely related to the ability to ask questions and create a relationship with the patient.
Studies show that between 60% and 80% of the information needed to establish the primary diagnosis are obtained during the interview with the patient.
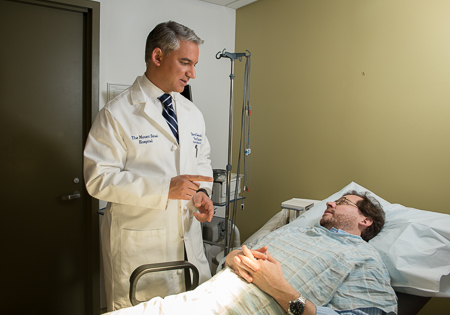
Why proper communication is crucial:
- information exchange;
- mutually accepted decisions;
- better understanding;
- building trust.
The physician is obligated too:
- concentrate this whole attention on the patient;
- creating an environment that protects the dignity of the patient;
- confidentiality (non-disclosure of intimate patient information to others);
- permanent concern for the well-being of the patient;
- respecting the rights of the patient or his / her family.
Patient Obligations:
- establishing a list of specific questions he/she wants to ask the doctor;
- if necessary, designate a family member or other trusted person to represent him/her in discussion with the doctor;
- open dialogue with the doctor;
- presenting as objectively as possible the symptoms he/she experiences;
- be utterly truthful in everything the patient is information the doctor off.
When all of the above obligations aren’t respected by either of the parties involved and the overall physician-patient relationship is deficient so of the consequences may include: frustration, anger, accusations, an increased number of tests or even getting a different opinion from another doctor.
And not only the patient can experience feelings of frustration or anger, but also the doctor who fails to achieve the patient’s healing.
Online communication and information
The Physician-Patient talks shouldn’t stop only with the traditional face-to-face discussions at the clinic. It can also include e-mail exchanges, phone talks, but also direct online chats via messager apps.
Doctors may also suggest different online resources where the patient can read more about specific conditions and even join special forums and online support groups where people with the same illness can help and support each other.
Until recently, during the consultations, the doctor was solely responsible for holding the scientific information. Now, with the ease with which such information can be obtained, patients can play an active role in the decision-making.
Of course, there is enormous concern over the certain accuracy content found online may have from a medical perspective. But this is why your doctor needs to play an essential role in all of this right from the start, guiding you into the right direction and helping you with approved online information.
Leaving everything in the hands of the patient regarding medical information can have disastrous consequences like scaring the patient or even giving the patient false hope.
Communicating the diagnosis
Disclosing the diagnosis to the patient, especially when it comes to incurable illnesses, is one of the problematic aspects of communication between the doctor and the patient.
Many doctors still believe that being faced with a grueling diagnosis, many patients may stop fighting the disease, getting depressed and overall losing the battle with the illness.
So, in the end, it is all about the doctor’s ability to sensitively attenuated the mental collision such a diagnosis can have on the patient while staying truthful.
Before communicating the diagnosis, it is good for the doctor to know as much as possible about his patient, about his life, his values, his abilities and his mental strength. Thus, when dealing with a terrible diagnosis, the news should come encouragingly, emphasizing what the patient could do to improve his condition.
For most doctors, it is all the more difficult to talk openly about when the diagnosis and the prognosis are reserved, and the patient is very young. Of course, the doctor can call on a psychologist to help with a communication strategy.
Lack of information creates confusion
One of the most significant issues with all Patient-Physician relationships is the lack of communication and how this void of knowledge creates confusion for both parties, but it can be especially bad for the patient.
When the patient does not receive the desired information, different reactions can be expected. The patient may be unhappy and then call another doctor. There is a category of patients who are “shopping” for doctors, gathering multiple investigations and a massive file of different treatments and test results.
The ambiguity of a discussion with a doctor can scare a patient. The patient may get a false impression that it’s something serious, maybe incurable, and the doctor hides it. The patient may start he can start looking for evidence to support his hypothesis and will interpret every symptom, every condition, and implement a self-diagnostic. All of this can be extremely dangerous. This is why physicians need to be very clear and leave no room for ambiguity when talking to the patient.

